Delamanid
- CAS NO.:681492-22-8
- Empirical Formula: C25H25F3N4O6
- Molecular Weight: 534.48
- MDL number: MFCD18251539
- SAFETY DATA SHEET (SDS)
- Update Date: 2026-04-09 22:57:55
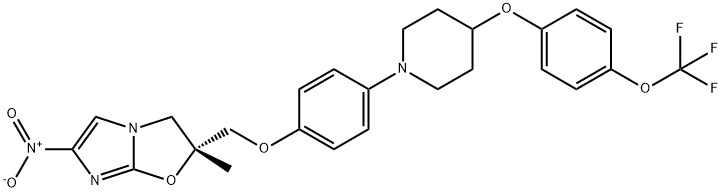
What is Delamanid?
Absorption
Following a single oral dose administration of 100 mg delamanid, the peak plasma concentration was 135 ng/mL . Steady-state concentration is reached after 10-14 days . Delamanid plasma exposure increases less than proportionally with increasing dose. In animal models (dog, rat, mouse), the oral bioavailability of delamanid was reported to be 35%–60% . The absolute oral bioavailability in humans is estimated to range from 25 to 47% . Oral bioavailability in humans is enhanced when administered with a standard meal, by about 2.7 fold compared to fasting conditions because delamanid exhibits poor water solubility .
Toxicity
While there have been no cases of delamanid overdose, some adverse reactions were observed at a higher frequency and the rate of QT prolongation increased in a dose-related manner. Treatment of overdose should involve immediate measures to remove delamanid from the gastrointestinal tract and supportive care as required. Frequent ECG monitoring should be performed .
Studies of genotoxicity and carcinogenic potential reveal no significant effects on humans. Delamanid and/or its metabolites have the potential to affect cardiac repolarisation via blockade of hERG potassium channels. During repeat-dose studies in dogs, foamy macrophages were observed in lymphoid tissue of various organs with delamanid treatment although clinical relevance of this finding was not established. Repeat-dose toxicity studies in rabbits revealed an inhibitory effect of delamanid and/or its metabolites on clotting factors II, VII, IX, and X via inhibition of vitamin K production . Embryo-fetal toxicity was observed at maternally toxic dosages in reproductive studies involving rabbits .
Description
Marketed by Otsuka, delamanid was approved in both the European Union and Japan in 2014 as part of combination therapies for multi-drug resistant tuberculosis (TB). Because delamanid exhibited no adverse drug–drug interactions, it has found utility as a combination therapy with standard antiretroviral drugs indicated for TB. Delamanid blocks mycolic acid biosynthesis in Mycobacterium tuberculosis, which allows its cell wall to be penetrated by small molecule antivirals.
The Uses of Delamanid
Delamanid is a novel anti-tuberculosis medication that inhibits mycolic acid synthesis and shows potent in vitro and in vivo activity against drug-resistant strains of Mycobacterium tuberculosis.
Background
Delamanid is an anti-tuberculosis agent derived from the nitro-dihydro-imidazooxazole class of compounds that inhibits mycolic acid synthesis of bacterial cell wall . It is used in the treatment of multidrug-resistant and extensively drug-resistant tuberculosis (TB) in a combination regimen. Emergence of multidrug-resistant and extensively drug-resistant tuberculosis creates clinical challenges for patients, as the disease is associated with a higher mortality rate and insufficient therapeutic response to standardized antituberculosis treatments as Isoniazid and Rifampicin. Multidrug-resistant tuberculosis may also require more than 2 years of chemotherapy and second-line therapies with narrow therapeutic index . In a clinical study involving patients with pulmonary multidrug-resistant tuberculosis or extensively drug-resistant tuberculosis, treatment of delamanid in combination with WHO-recommended optimised background treatment regimen was associated with improved treatment outcomes and reduced mortality rate . Spontaneous resistance to delamanid was observed during treatment, where mutation in one of the 5 F420 coenzymes responsible for bioactivation of delamanid contributes to this effect . Delamanid is approved by the EMA and is marketed under the trade name Deltyba as oral tablets. It is marketed by Otsuka Pharmaceutical Co., Ltd (Tokyo, Japan).
Indications
Indicated for use as part of an appropriate combination regimen for pulmonary multi-drug resistant tuberculosis (MDR-TB) in adult patients when an effective treatment regimen cannot otherwise be composed for reasons of resistance or tolerability .
Definition
ChEBI: Delamanid is a member of piperidines.
Pharmacokinetics
The minimum inhibitory concentrations (MIC) of delamanid against Mycobacterium tuberculosis isolates ranges from 0.006 to 0.024 g/mL . Among non-tuberculosis mycobacteria, delamanid has in vitro activity against M. kansasii and M. bovis . Delamanid has no in vitro activity against Gram negative or positive bacterial species and does not display cross-resistance to other anti-tuberculosis drugs . In murine models of chronic tuberculosis, the reduction of M. tuberculosis colony counts by delamanid was demonstrated in a dose-dependent manner . Repeated dosing of delamanid may cause QTc-prolongation via inhibition of cardiac potassium channel (hERG channel), and this effect is mostly contributed by the main metabolite of delamanid, DM-6705 . Animal studies indicate that delamanid may attenuate vitamin K-dependent blood clotting, increase prothrombin time (PT), and activated partial thromboplastin time (APTT) .
Clinical Use
Treatment of multi-drug resistant tuberculosis
Synthesis
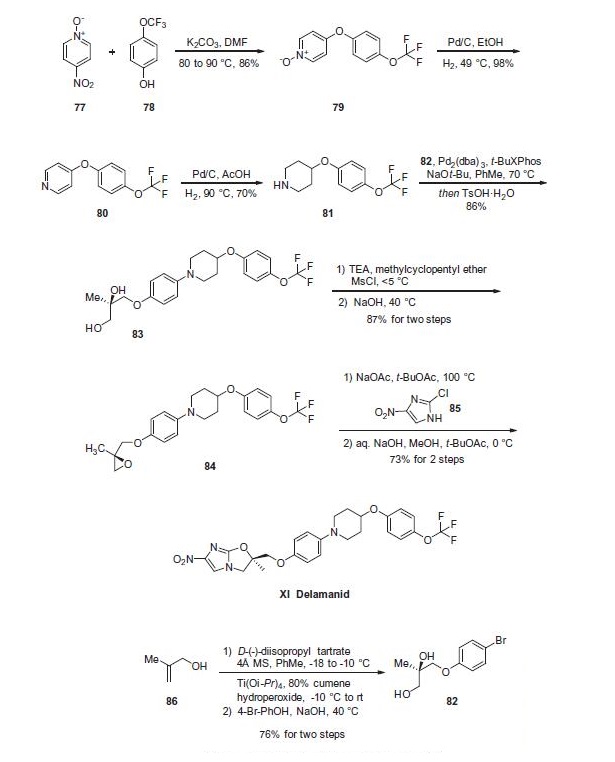
Piperidine 81 was concurrently prepared by first generating biaryl ether 79, which arose from a substitution reaction between pyridine N-oxide 77 and phenol 78 that proceeded in 86% yield. Next, removal of the N-oxide functionality by means of catalytic hydrogenation under mild pressure and neutral conditions afforded diaryl ether 80 in excellent yield. Reduction of the pyridine to the corresponding piperidine (81) was affected through the use of catalytic hydrogenation as well, this time under acidic conditions and elevated pressures relative to the N-oxide reduction. At this juncture, subjection of piperidine 81 to Buchwald¨C Hartwig conditions in the presence of diol subunit 82 delivered diol 83. A two-step elimination to deliver enantiopure epoxide 84 set the stage for an interesting cascade reaction to arrive at delamanid (XI) directly?a the initial alkylation of the epoxide by imidazole 85 proceeded under basic conditions with sodium acetate which then underwent an intramolecular nucleophilic substitution reaction by the liberated alcohol on the pendant imidazole chloride in the presence of sodium hydroxide. The reaction sequence proceeded in 73% yield to provide delamanid (XI) as a free base.
Drug interactions
Potentially hazardous interactions with other drugs
Analgesics: increased risk of ventricular arrhythmias
with methadone
Anti-arrhythmics: increased risk of ventricular
arrhythmias with amiodarone and disopyramide
Antibacterials: possible increased risk of ventricular
arrhythmias with clarithromycin, erythromycin
and moxifloxacin; increased risk of ventricular
arrhythmias with pentamidine; concentration
reduced by rifampicin
Antidepressants: possible increased risk of
ventricular arrhythmias with tricyclics.
Antiepileptics: avoid with carbamazepine.
Antipsychotics: increased risk of ventricular
arrhythmias with droperidol, haloperidol,
phenothiazines that prolong the QT interval and
pimozide.
Antivirals: increased risk of ventricular arrhythmias
with saquinavir
Beta-blockers: increased risk of ventricular
arrhythmias with sotalol.
Cytotoxics: increased risk of ventricular arrhythmias
with arsenic trioxide and possibly vinblastine,
vincristine, vindesine, vinflunine and vinorelbine
Domperidone: possible increased risk of ventricular
arrhythmias.
Metabolism
Delamanid predominantly undergoes metabolism by albumin and to a lesser extent, CYP3A4. . The metabolism of delamanid may also be mediated by hepatic CYP1A1, CYP2D6, and CYP2E1 to a lesser extent [31966]. Four major metabolites (M1–M4) have been identified in plasma in patients receiving delamanid where M1 and M3 accounts for 13%–18% of the total plasma exposure in humans . While they do not retain significant pharmacological activity, they may still contribute to QT prolongation . This is especially true for the main metabolite of delamanid, M1 (DM-6705) .
Delamanid is predominantly metabolized by serum albumin to form M1 (DM-6705) via hydrolytic cleavage of the 6-nitro-2,3-dihydroimidazo[2,1-b] oxazole moiety. The formation of this major metabolite is suggested to be a crucial starting point in the metabolic pathway of delamanid . M1 (DM-6705) can be further catalyzed by three pathways. In the first metabolic pathway, DM-6705 undergoes hydroxylation of the oxazole moiety to form M2 ((4RS,5S)-DM-6720), followed by CYP3A4-mediated oxidation of hydroxyl group and tautomerization of oxazole to an imino-ketone metabolite, M3 ((S)-DM-6718) . The second metabolic pathway involves the hydrolysis and deamination of the oxazole amine to form M4 (DM-6704) followed by hydroxylation to M6 ((4R,5S)-DM-6721) and M7 ((4S,5S)-DM-6722) and oxidation of oxazole to another ketone metabolite, M8 ((S)-DM-6717) . The third pathway involves the hydrolytic cleavage of the oxazole ring to form M5 (DM-6706) .
Metabolism
Delamanid is mainly metabolised in plasma by albumin and to a lesser extent by CYP3A4. The complete metabolic profile of delamanid has not yet been elucidated. The identified metabolites do not show anti-mycobacterial activity but some contribute to QT prolongation, mainly DM-6705.
Properties of Delamanid
| Melting point: | 195-196℃ |
| Boiling point: | 653.7±65.0 °C(Predicted) |
| Density | 1.45 |
| storage temp. | Hygroscopic, -20°C Freezer, Under inert atmosphere |
| solubility | Chloroform (Sparingly), Ethyl Acetate (Slightly, Sonicated) |
| form | Solid |
| pka | 3.99±0.20(Predicted) |
| color | Off-White to Light Yellow |
| Stability: | Hygroscopic |
Safety information for Delamanid
Computed Descriptors for Delamanid
New Products
3-azanyl-3-phenyl-propanoic acid 3-AMINO-3-(2-METHYLPHENYL)PROPANOIC ACID 3-AMINO-3-M-TOLYL-PROPIONIC ACID Nitroso Irbesartan N-Nitroso Nortriptyline 1-nitro-3,5-dimethyl adamantine (NMEM) 3-(2-aminoethyl) benzene sulfonamide Nabumetone Impurity 5 2,2-dibromo-1-cyclopropyl-2-(2-fluorophenyl)ethan-1-one 4-dimethylaminopyridine 3-Bromo-2-Methyl-5-Nitropyridine 2-Chloro Isonicotinic acid methyl ester 2-(Ethoxymethylene)propanedinitrile 5-Bromo-3-Methyl-2-Pyridinecarboxylic acid 5-Chloro-pyridine-2-carboxylic acid amideRelated products of tetrahydrofuran
You may like
-
 Delamanid CAS 681492-22-8View Details
Delamanid CAS 681492-22-8View Details
681492-22-8 -
 3646-50-2 3-azanyl-3-phenyl-propanoic acid 98+View Details
3646-50-2 3-azanyl-3-phenyl-propanoic acid 98+View Details
3646-50-2 -
 3646-50-2 3-azanyl-3-phenyl-propanoic acid 98+View Details
3646-50-2 3-azanyl-3-phenyl-propanoic acid 98+View Details
3646-50-2 -
 68208-16-2 98+View Details
68208-16-2 98+View Details
68208-16-2 -
 3-AMINO-3-M-TOLYL-PROPIONIC ACID 98+View Details
3-AMINO-3-M-TOLYL-PROPIONIC ACID 98+View Details
68208-17-3 -
 3646-50-2 3-azanyl-3-phenyl-propanoic acid 98+View Details
3646-50-2 3-azanyl-3-phenyl-propanoic acid 98+View Details
3646-50-2 -
 68208-16-2 98+View Details
68208-16-2 98+View Details
68208-16-2 -
 3-AMINO-3-M-TOLYL-PROPIONIC ACID 98+View Details
3-AMINO-3-M-TOLYL-PROPIONIC ACID 98+View Details
68208-17-3

